By Rachael Schultz
For something that literally half the population will go through, menopause still feels oddly mysterious. Many of us were never really taught when it starts, how long it lasts, or how to recognize the early signs. And because it’s long been stigmatized with “getting old,” we’re often caught off guard when our bodies begin to change in our 30s, 40s, or 50s.
“Every individual has a life cycle. Women often have a negative association with the change in their ovaries, but it’s really just the life cycle of our bodies,” says Gloria A Bachmann, MD, professor of obstetrics and gynecology and medicine and co-director of the Women’s Health Institute at Rutgers University.
Menopause is as natural as getting your period for the first time — and often comes with more changes. The more you understand what’s happening under the surface, the more empowered you’ll be to manage symptoms, protect your long-term health, and advocate for the care and support you need.
Whether you’re going through menopause as we speak or wondering when it’s going to hit you, now feels like a great time to dive into what happens to women’s bodies during this phase of life.
The Phases of Menopause
Menopause is a completely natural part of your biology, Dr. Bachmann emphasizes. Whether it begins on its own or is brought on by a procedure like a hysterectomy, it’s a transition — a new stage of life that every woman who lives long enough will move through.
Here’s the basic idea: Women are born with all the eggs they’ll ever have. Once you begin menstruating, your body releases an egg every month — that’s known as ovulation. When the egg releases, your body also releases estrogen and progesterone, two key hormones that regulate your menstrual cycle, prepare you for pregnancy, and influence everything from your bones to your brain.
Eventually, your limited supply of eggs (follicles) begins to dwindle and stop functioning. When there are no longer enough to spark ovulation, your body starts shifting into the transition we know as menopause.
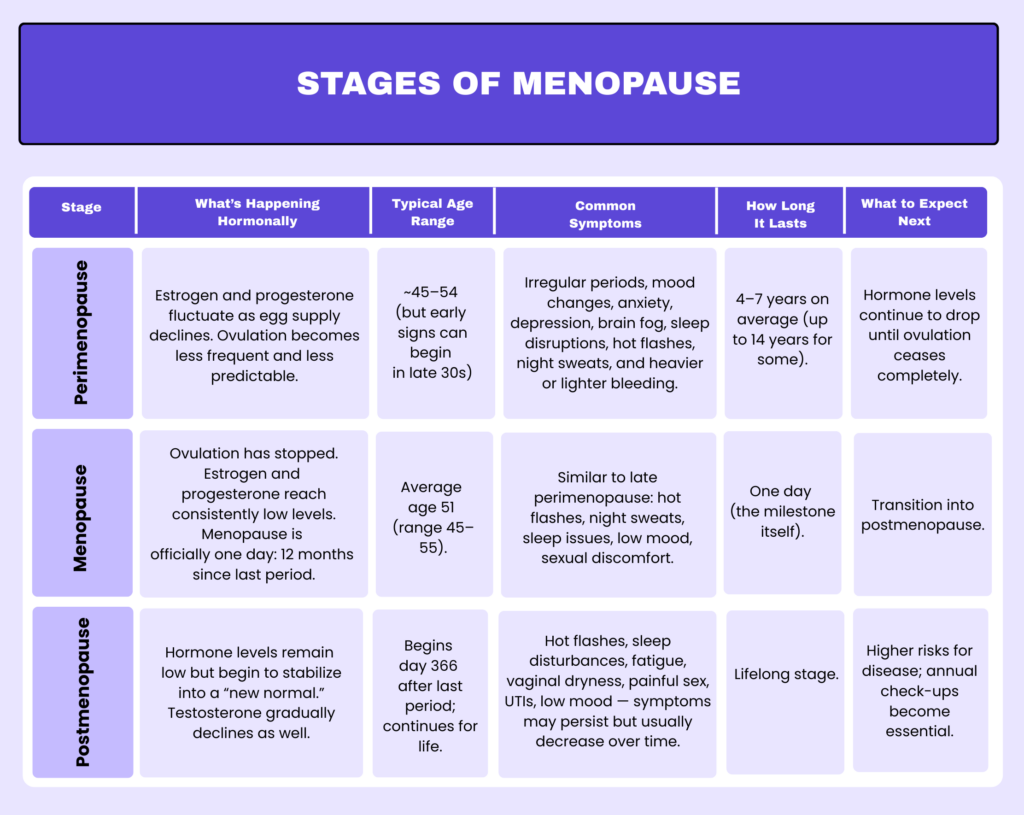
The transition is generally divided into three phases: before (peri), during (menopause), and after (post).
Related: Why You Should Lift Weights If You’re Over 40
1. Perimenopause
Perimenopause, or the “menopausal transition,” is the period of time when your body stops releasing an egg on a predictable 21–35 day cycle. Menopause is defined as going a full year without a period, but perimenopause is the span of time before this. During this stage, your viable egg stores begin to decline, causing your estrogen and progesterone levels to fluctuate from month to month.
Most women start perimenopause sometime between 45 and 54 years old. That said, Dr. Bachmann points out that many women begin to notice changes in their menstrual cycle — less frequent ovulation or heavier bleeding — in their mid to late 30s. It can last up to 14 years, but most women experience it for 4 to 7 years.
Perimenopause can be surprisingly hard to recognize. A 2025 study analysis found that 55 percent of women ages 30 to 35 report moderate to severe symptoms tied to menopause. These early signs — things like anxiety, depression, irritability — often show up before the classic hot flashes and night sweats.
In the early stages, Dr. Bachmann says, most women start to have less-regular periods — maybe one every three months. At this point, your hormones are working to compensate for the low number of remaining ovarian follicles, which can lead to mild symptoms from shifting levels: mood shifts, sleep disturbances, and even brain fog.
As you move into the later stage of perimenopause, your estrogen levels drop so low that your ovaries and pituitary glands can’t produce enough hormones to balance things out. At this point, your body isn’t releasing an egg each month, and the hormonal shifts become more pronounced.
This is when symptoms become more noticeable and more frequent. Bone mineral loss becomes detectable. Often, the vasomotor symptoms set in — hot flashes, night sweats, a rapid heartbeat. Sleep takes a hit, too, thanks to the roller coaster of hormones and body temperatures.
2. Menopause
Although we tend to use the term “in menopause” to describe everything from perimenopause to post-menopause, medically, menopause is actually only a single day. It’s the point that marks 12 consecutive months without a period. It marks the moment your ovaries have officially stopped releasing eggs.
In the U.S., the average age of menopause is 51 years old, with most women naturally hitting this marker between ages 45 and 55.
This stage looks very similar to late-stage perimenopause. Your body has already gone months without its monthly hormone cycle, so it’s really just an official marker of your new norm.
3. Postmenopause
Postmenopause begins on day 366 after your last period, and continues for the rest of your life. At this point, your hormone levels are persistently lower than they have been in your adult life. In the early part of this stage, though, your body is still figuring out how to settle into its new normal — your hormones are adjusting, and your system is recalibrating right along with them.
Even after menopause, symptoms like hot flashes, sleep disruptions, fatigue, and low mood, can persist. Testosterone levels, which remain steady during perimenopause, start to decline during this stage, contributing to sexual dysfunction, anxiety, depression, and an increased likelihood of hot flashes.
That said, as your hormones settle into their new post-fertile norm, your body and brain start to adapt. Research shows that body temperature changes and, to some extent, sleep disturbances often ease within one to six years. Mood swings generally level out, too.
However, without treatment, some side effects are here to stay: Long-term estrogen loss increases the likelihood of weight gain and may lead to ongoing vaginal dryness, painful sex, and recurring urinary track infections (UTIs).
Your risk for certain diseases also rises after menopause — including heart disease, osteoporosis, type 2 diabetes, dementia and Alzheimer’s, obesity, and sexual dysfunction.
That’s why it’s absolutely crucial to stay on top of your annual check-ups after you’ve gone through menopause, Dr. Bachmann says.
What exactly is happening in your body during menopause?
Menopause sounds simple: once your ovaries run out of egg stores, you stop ovulating, which means your body no longer releases its monthly cycle of estrogen and progesterone, along with other key hormones like testosterone, follicle-stimulating hormone (FSH), and luteinizing hormone (LH).
But what isn’t simple is how many biological systems in your body these hormones influence.
In women, estrogen helps regulate metabolism, increase blood flow to the brain, and affects how quickly and efficiently brain neurons grow, connect, and fire. It also keeps your heart working optimally and, along with progesterone and testosterone, helps regulate your nervous system.
What are the most common symptoms?
Without the steady supply of estrogen your body has been working with for 25 to 45 years, nearly every system in the body is affected, though the specifics look different for each woman.
About 85% of women experience symptoms, but the mix varies widely. It’s truly a complete grab-bag from woman to woman.
Common symptoms include:
- Issues with mental clarity, like brain fog and slower recall
- Irritability and mood changes
- Hot flashes
- Night sweats
- Depression
- Anxiety
- Weight gain
- Sexual dysfunction, including vaginal dryness, painful sex, and UTIs
After menopause, your risk for certain diseases also rises, including:
- High blood pressure
- Cardiovascular disease
- Obesity
- Type 2 diabetes
- Osteoperosis
- Alzheimer’s and dementia
Symptoms also tend to shift over time. Research shows psychological menopausal symptoms — anxiety, depression, irritability — are more common among women in their 30s, and appear well before the physical symptoms. After age 51, the most common symptoms include sexual dysfunction, bladder issues, and vaginal dryness.
Related: Menopause and Bone Loss
When should you see your doctor?
Check in with your doctor about menopause as early as possible, Dr. Bachmann advises. If your periods become irregular or unusually heavy, or you start to experience any of the symptoms mentioned above out of the blue, talk to your primary care provider or OB-GYN.
Dr. Bachmann also recommends making two appointments from the start — one to discuss what you’re experiencing, and another to run bloodwork and check your hormone levels to confirm you’re in perimenopause. At the very least, make your follow-up appointment before you leave the doctor’s office.
You want to know if you’re in perimenopause as early as possible because research shows that at least 20% of women say their menopause symptoms significantly impact their quality of life. A 2023 Dutch study found that among the 80% of women who experienced symptoms during perimenopause, a significant number reported that those symptoms interfered with their work, impacted their health, and left them feeling noticeably more emotionally exhausted.
The earlier you bring this up to your doctor, the earlier you can start treatment, Dr. Bachmann says. We’ve long known that hormone therapy is super effective at treating menopausal symptoms. But it can also help lower some of the long-term risks that rise after menopause. A new study presented at the 2025 Annual Meeting of The Menopause Society reports that women who started estrogen therapy at least 10 years before menopause had significantly lower odds of developing breast cancer, heart attacks, and strokes compared with women who started after menopause or didn’t use hormone therapy at all.
How to support your body during menopause
Your primary care doctor or OB-GYN will help guide you toward the options that are best for you.
According to Dr. Bachmann, hormone therapy is the most effective treatment for both peri- and postmenopausal symptoms. Typically delivered as estrogen alone or a combination of estrogen and progestin, it replaces the monthly hormonal supply your body no longer produces. Hormone therapy is highly effective and carries a low risk to younger women’s health. It can be prescribed locally, transdermally, or orally — each approach targeting specific symptoms — so talk to your doctor about what you’re experiencing and which form may be the best fit.
Additionally, small changes to your daily habits and lifestyle can help ease many common symptoms. “You want to feel your best so nothing interferes with your life and all the other activities we’re all involved with,” Dr. Bachmann says. These include:
- Dress smarter and control your temperature. Vasomotor symptoms — sweating, flushing, a rapid heartbeat — can be hard to contend with, but layering breathable fabrics and keeping your home cooler, especially at night, can help. Many women also find relief by placing a cold pack under their pillow.
- Learn your triggers. Spicy foods, alcohol, and coffee are all common culprits behind hot flashes. Knowing what triggers your symptoms is key to minimizing their disruptions.
- Eat whole foods and move more. Focusing on your diet and activity can help manage your weight.
- Do your Kegels. Lower estrogen levels can cause the muscles and tissue of the pelvic floor to lose strength and elasticity, contributing to sexual discomfort and urinary incontinence. Kegel exercises help to offset this.
- Get regular check-ups. Your risk for major health conditions increases after menopause, so it’s important to get a full preventive health visit at least once a year with your primary care doctor. If they don’t do a gynecological checkup, you should also see your OB-GYN annually.
Related: Thriving Through Menopause
Navigating menopause with confidence
Menopause is a natural transition, but it can bring real changes to how you feel day to day. Understanding what’s happening in your body — and getting support early — can make the experience far more manageable. With the right tools, care, and lifestyle adjustments, you can navigate this stage feeling informed, supported, and empowered.
Stronger Together
At Every Stage
Join a global community that supportings each other through every stage of life — with movement, mindset, and science on our side.





